Tongue Ties
Understanding Tongue-Tie: What You Need to Know
Do you experience snoring, teeth grinding or clenching, headaches, jaw pain, or even migraines? Have you noticed difficulty pronouncing certain words, issues related to ADHD or ADD, or general body tension? Do you breathe primarily through your mouth? If so, you may have a condition known as tongue-tie.
A tongue-tie is a condition that occurs when the frenum—the tissue connecting your tongue to the floor of your mouth—is abnormally tight or restrictive. This tissue is present in everyone, but for some, it’s too tight, leading to a variety of issues both inside the mouth and throughout the body.
Why Does A Tongue-Tie Matter?
The way your tongue is attached to the mouth’s floor plays a significant role in facial development and the proper functioning of the mouth during activities like breathing, swallowing, and speaking.
The lingual frenum (also called the frenulum) is the tissue that runs under your tongue and connects it to the mouth's floor. For many, this tissue may be too tight or restrictive, a condition referred to as a tongue-tie, restricted lingual frenum, or tethered oral tissue. This restriction limits the tongue’s movement and prevents it from resting in the correct position, leading to several functional issues and symptoms that can vary in severity.
The position of the tongue is essential for overall health. Ideally, the tongue should rest comfortably against the roof of the mouth (front to back), providing structural support for the upper jaw. Proper tongue positioning helps with the alignment of teeth and promotes optimal facial development. However, a tongue-tie can restrict the tongue from reaching the palate, which results in improper positioning and inefficient function.
People with tongue-tie often mouth breathing (sometime without realizing it), which can lead to a wide range of issues such as chronic jaw pain, sleep apnea, facial pain, headaches, teeth grinding, and orthodontic concerns. Research indicates that children with tongue-tie are at a higher risk of developing sleep apnea, airway problems, and their facial and cranial development is impacted.
How Can Myofunctional Therapy Help?
If you have a tongue-tie, a simple procedure called a frenectomy can help. During your myofunctional assessment, I will evaluate whether this procedure is indicated. If surgery is needed, it's important to undergo specific exercises both before and after the procedure to maximize results.
Myofunctional therapy plays an essential role in strengthening and stabilizing the tongue’s movement to prevent it from re-attaching to its original, restricted position. Re-training the tongue is a vital step in the recovery process. When you have a tongue-tie it limits range of motion and leads to compensations of other muscles, creating dysfunction. Once this restricted is released, we will work through a series of exercises to help re-train correct function.
I will assist you in coordinating your exercise sessions with your doctor performing the procedure to ensure optimal timing and results.
Anterior vs. Posterior Tongue Tie
There are two primary types of tongue-tie: anterior and posterior.
Anterior tongue-tie is more apparent, as it can be easily identified when the tongue is lifted. In this case, the tissue underneath the tongue is tightly connected to the floor of the mouth, limiting the tongue’s range of motion.
Posterior tongue-tie, on the other hand, can be more challenging to detect and diagnose. This type is often symptom-based, and the restriction is located toward the back of the tongue. Because other muscles in the face and mouth may compensate for this limitation, it can lead to pain and tension in the neck, jaw, and face, as well as issues like clenching, grinding, TMJ disorders, and sleep apnea.
Speech and Tongue-Tie
Tongue-tie can impact speech, particularly in the pronunciation of certain sounds like "R" and "L." These sounds require specific tongue movements, which can be difficult to produce if the tongue cannot move freely due to the restriction caused by a tongue-tie. When you are tongue-tied, your tongue isn’t able to elevate to the roof of the mouth to create those sounds easily.
How We Assess and Treat Tongue-Tie
When you visit for an evaluation, your myofunctional therapist will assess your tongue’s mobility and identify any restrictions. If a tongue-tie release is recommended, you'll be referred to a specialized surgeon experienced in treating tongue-tie.
The release procedure typically occurs midway through therapy after you have built up enough muscle coordination and strength around the frenulum. After the procedure, we will work together to continue strengthening and improving the function of the newly released tongue, helping you work towards optimal oral function.
-
Several factors are leading to a renewed interest in tongue ties:
An increased focus on the benefits of breastfeeding in the 1990s led many parents to search for answers to challenges such as poor latch, painful nursing, insufficient milk intake, and the need for constant nursing.
A newer hypothesis that has emerged in the last several years talks about the increased use of folic acid starting in the 1980s to effectively prevent birth defects may have had the unintended consequence of a thickening of structures at the midline of the body, including tongue and lip ties.
In 1999 and 2004, the medical community was introduced to the idea that a tongue does not need to extend all the way to the tip to cause problems in feeding, growth, and development. Since then, several case reports and large research studies have described a posterior tongue tie or posterior tongue restriction that can cause problems in babies and children, which become progressively worse as those children grow up into adults.
Our society’s ability to communicate with many diverse communities allow individuals with symptoms that were previously unable to find underlying causes are now able to find that information for themselves.
The continued advancement of communication and educational technology allows healthcare providers to seek out and find answers to problems their patients are experiencing, and then share the successes and failures with those treatments.
Healthcare providers finding success in treating patients are willing to share that knowledge with other providers through easy to access learning libraries, social media, digital courses, and written materials, increasing access to this information at an accelerated pace. In the past, the sharing of knowledge was often limited to the immediate area. Now, practitioners are able to learn from other healthcare providers in Alabama, Oregon, California, Ireland, Australia, and other areas around the world from their homes or offices, reducing the need to travel around the world to find world class education in current medical trends.
The increase in knowledge and awareness does not explain the whole story as to why tongue tie has increased. Genetic and epigenetic causes may have additional explanations as to why it is more prevalent in our communities. Genetic mutations over the last century coupled with a change in lifestyle, diet, exposure to chemicals, and radiation has an impact on the DNA that is passed from one generation to the next. Those gene mutations can be passed along to children and may have led to a larger prevalence of tongue tie in the population. We cannot go back and do studies on the tissue, but several researchers have studied the bones of previous populations and we can conclude that the tongue restrictions that lead to our living generations dental malocclusion and smaller airway may not have been so prevalent.
A Modern Understanding of Tongue-Tie
The understanding of how to identify a tongue-tie has evolved over time. In the past, a simple, one-dimensional understanding of tongue-tie (ankyloglossia) was used. Today, we have a more comprehensive understanding of how the frenulum, fascia, muscle attachments, and mobility all contribute to normal function.
The current definition of tongue-tie, as defined by the International Affiliation of Tongue-Tie Professionals (IAAP), is an embryological remnant of tissue in the midline between the underside of the tongue and the floor of the mouth that restricts normal tongue movement.
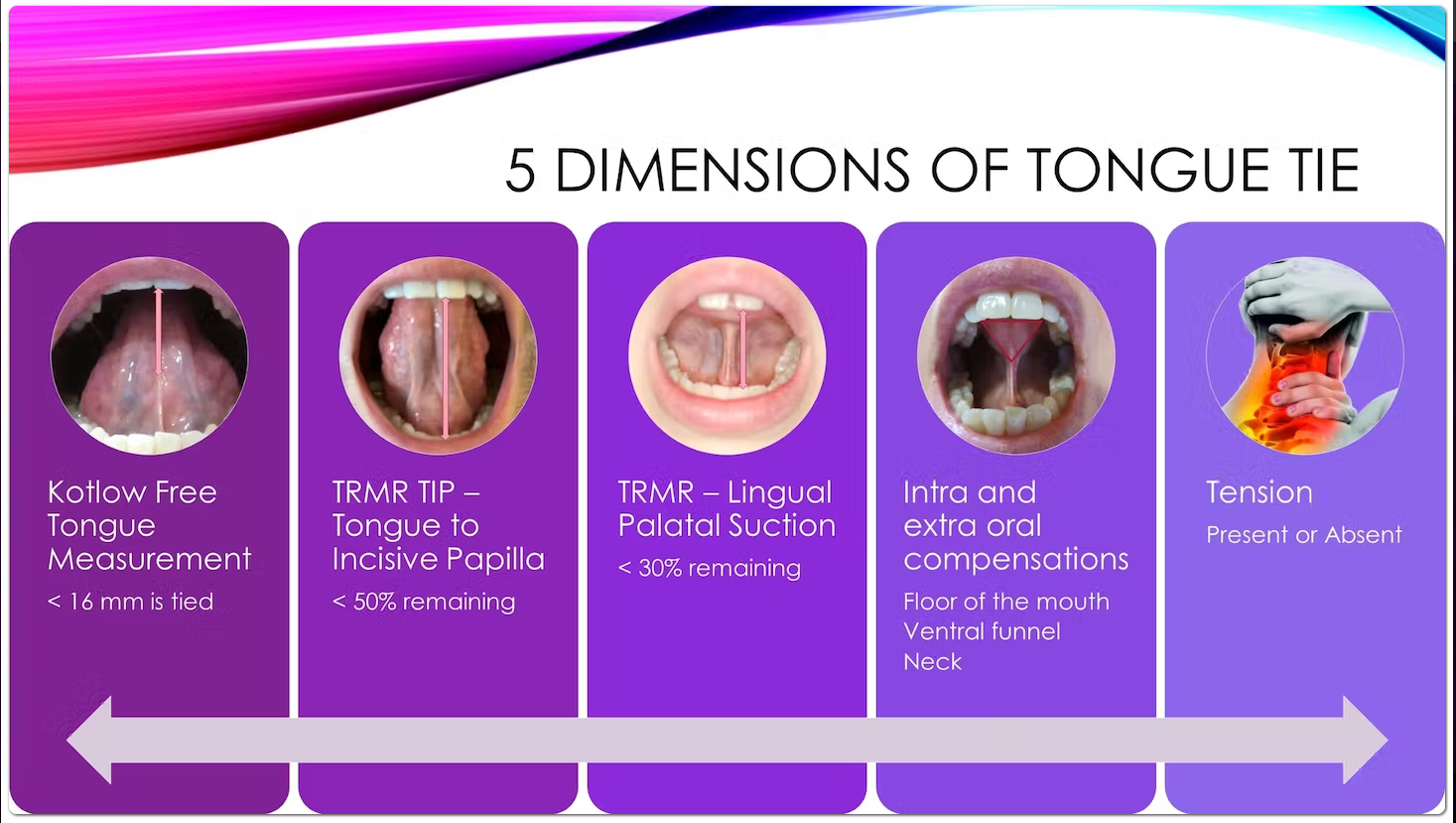
We now assess tongue-tie in five key dimensions:
How far you can stick out the tongue
How far you lift the tongue up to the incisive papilla, ”the spot” (just behind the upper back teeth with mouth open)
How far you can open your mouth while your tongue is fully suctioned to the roof of your mouth
How much the floor of the mouth, neck, and other muscles help you to suction your tongue or lift your tongue to the spot
Muscle tension caused by the first three
Additional Resources
Dr. Zaghi, one of the world leaders in tongue ties: https://www.zaghimd.com/tongue-tie